Few decisions in practice management carry more long-term financial weight than how you manage your revenue cycle. Build an in-house team and invest in the infrastructure to run it? Or hand the function to a specialized RCM partner and redirect that energy toward patient care?
In 2026, the landscape has shifted. Technology costs have changed, billing complexity has increased, and the talent market for experienced coders and billing specialists remains tight. Here’s an honest breakdown of what both options actually look like — and how to decide what’s right for your practice.
The Core Question — Build or Buy?
At its core, this is a classic build-vs-buy decision. In-house billing means building and maintaining the capability internally. Outsourced RCM means purchasing that capability from a specialist. Both can work. The question is which one produces better outcomes at a lower total cost for your specific practice type, size, and complexity.
What In-House Medical Billing Really Costs
Many practices underestimate the true cost of in-house billing. The calculation usually starts with salary — but stops too early. A full-cost view includes:
- Salaries and benefits for billing staff, coders, and AR follow-up personnel.
- Ongoing training and continuing education to keep pace with annual code updates, payer policy changes, and compliance requirements.
- Billing and practice management software licenses.
- Management overhead — someone has to supervise the team, handle escalations, and manage vendor relationships.
- Revenue leakage from errors — which is harder to quantify but often significant. In-house teams without specialty-specific expertise consistently produce higher denial rates.
For a practice with two or three billing staff, total annual cost of ownership frequently exceeds $200,000 to $300,000 — before accounting for coverage gaps during vacations, turnover, or illness.
The right answer for your practice starts with an honest assessment of where your revenue cycle currently stands — and what it would actually take to improve it.
Co-Founder - Squadyen Healthcare Solutions
What Outsourced RCM Actually Delivers
A strong RCM partner doesn’t just process claims. The best partners bring:
- Specialty-specific coding expertise across ICD-10, CPT, and HCPCS code sets.
- Dedicated denial management teams that follow up on every denied claim — not just the high-value ones.
- Real-time reporting dashboards that give practice leadership visibility into denial rates, clean claim rates, AR aging, and collection performance.
- Proactive compliance monitoring to reduce audit risk.
- Scalability — as your practice grows or contracts, the service scales with you without headcount changes.
Most outsourced RCM pricing is structured as a percentage of collections or a per-claim fee, which aligns the vendor’s incentives with your outcomes. If they collect more, they earn more.
Head-to-Head Comparison
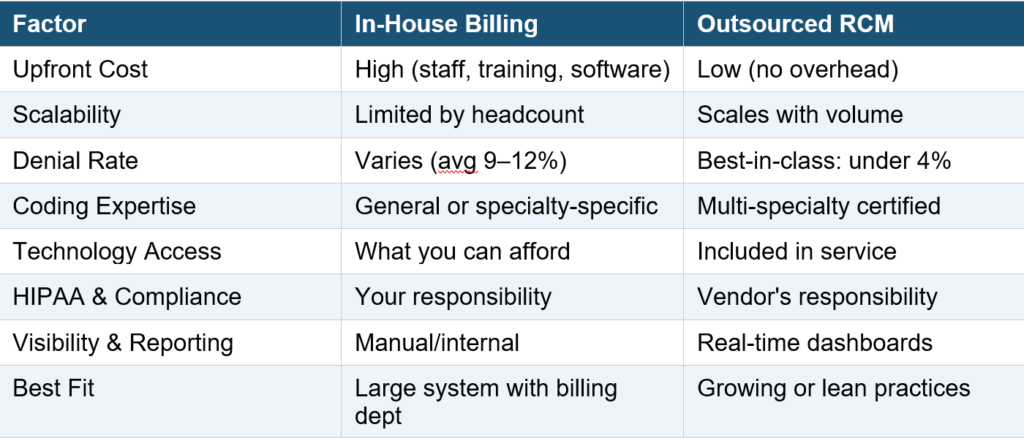
5 Signs It's Time to Outsource
If several of these apply to your practice, it’s worth having a serious conversation about transitioning to an outsourced model:
Your denial rate is consistently above 5% and hasn’t improved despite internal efforts.
AR days are trending upward and claims are regularly aging past 60 days without resolution.
You have lost billing staff recently and are struggling to backfill experienced replacements.
Your practice is expanding into a new specialty or adding payers, and the complexity is outpacing your team’s capacity.
You are spending significant leadership time managing billing operations rather than clinical strategy.
How to Evaluate an RCM Partner
Not all RCM companies deliver the same results. When evaluating potential partners, ask:
- What is your average denial rate across your client base? (Benchmark: under 5%)
- What is your average clean claim rate? (Target: above 95%)
- Do you have specific experience with our specialty and our primary payers?
- How do you report performance? What does a monthly reporting package look like?
- What are your SLAs for claim submission timelines and denial follow-up?
- Can you provide references from practices similar to ours in size and specialty?
A credible RCM partner will answer these questions directly and provide data to back up their claims. Vague answers are a red flag.
Common Objections — Answered Honestly
‘We’ll lose control of our billing.’ — Transparency, not control, is what matters. A good partner gives you more visibility into your revenue cycle performance than most in-house teams provide. Real-time dashboards and monthly reviews put you in a more informed position, not a less informed one.
‘It’s too expensive.’ — Compare the total cost of ownership, not just the service fee. When you factor in salary, benefits, training, software, and revenue leakage from a higher denial rate, outsourcing is frequently less expensive — especially for practices under 10 providers.
‘Our current team knows our patients.’ — Patient relationship management and billing are different functions. Your front desk and clinical staff can continue to own patient-facing interactions. Billing is a back-office function that doesn’t require face-to-face patient knowledge to execute well.
‘We tried outsourcing before and it didn’t work.’ — Poor results from one vendor don’t reflect the category. Ask specifically what went wrong — was it reporting transparency? Denial follow-up speed? Specialty expertise? Use those specific failure points as your evaluation criteria for the next partner.
There’s no universal answer to the build-vs-buy question in medical billing. Large health systems with robust infrastructure, dedicated revenue cycle departments, and strong internal training programs may be well-served by in-house operations. Growing practices, lean groups, and multi-specialty organizations frequently find that outsourcing delivers better financial outcomes at a lower total cost.
📌 📅 Book a Free 30-Minute RCM Health Check — Our team will benchmark your denial rate, AR days, and clean claim rate against industry standards and show you exactly where you stand.
